Nipah virus: What nurses need to know
What is Nipah virus?
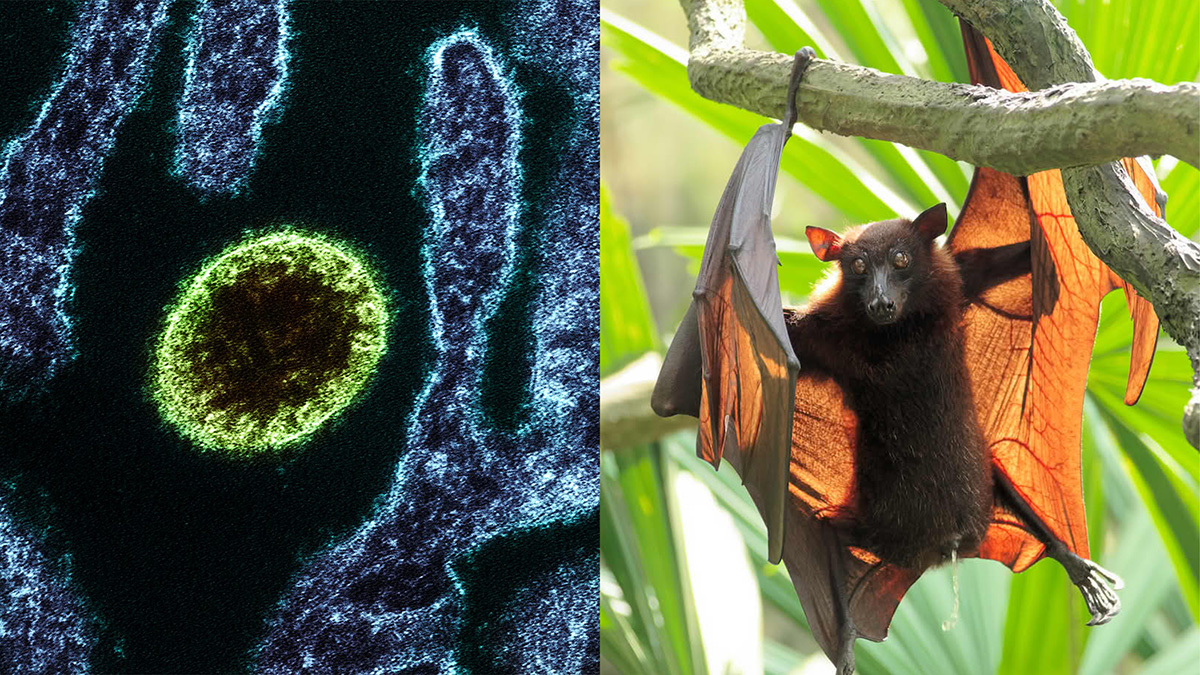
Nipah virus is a zoonotic virus, which means that it circulates in an animal reservoir (fruit bats) and can spread to infect livestock and humans. Nipah virus can also be transmitted from person to person. Nipah virus is one of the most lethal pathogens known to infect humans with a case fatality rate of 40 to 75 percent.
Hundreds of Nipah virus cases have been reported in Malaysia, Bangladesh, India, and a few other countries since the 1990s when it was first identified. Most of these cases have been in adults (89 percent), males (74 percent), and among livestock practitioners (68 percent).
Infection with Nipah virus can be difficult to distinguish from other infectious diseases and diagnosis requires lab testing. There are no approved drugs for Nipah virus. Treatment consists of supportive care. No vaccines exist, though a range of products are under different stages of development. Early detection and response are essential to control outbreaks.
What are the symptoms of Nipah virus infection?
Symptoms of Nipah virus typically begin with fever, symptoms involving the brain such as headache or confusion, and/or symptoms involving the lungs such as difficulty breathing or coughing. Other common initial symptoms include chills, fatigue, drowsiness, dizziness, vomiting, and diarrhea.
Disease progresses rapidly with Nipah virus. Any patient can develop severe disease, but progression is most associated with patients presenting with early neurological symptoms. Nipah virus can progress to encephalitis (brain swelling), which can quickly result in a coma, and frequently death.
For those that survive Nipah virus, most make a full recovery, but some will suffer long-term neurological damage.
There is evidence that some Nipah virus infections can be asymptomatic.
How is Nipah virus transmitted?
Transmission most frequently occurs from infected animals (bats or livestock) to humans but can also occur from person to person. Available data supports contact and aerosol transmission as modes of transmission for Nipah virus. The incubation period is three to 14 days, with some rare cases up to 45 days.
Risk factors for Nipah virus infection
The primary risk factor for Nipah virus infection is contact with infected or sick animals (69 percent of cases with known exposure). Other risk factors include exposure to infected individuals (26 percent) and exposure through date palm-related activities (5 percent).
Transmission via animals
The natural host of Nipah virus is fruit bats from the Pteropodidae family, which live in parts of Asia and Australia. Nipah virus typically does not cause disease among fruit bats.
Transmission to humans can occur from direct contact with infected bats or their saliva, urine, or other secretions. When food products, such as raw date palm syrup, are contaminated by bats, then consumed by humans, transmission can occur. Nipah virus can survive for days on sugar-rich solutions like fruit pulp.
Transmission of Nipah virus can also occur via infected animals where bats have contaminated animals’ feed or environments leading to infection among livestock such as pigs or horses. Humans interacting with infected livestock can become infected.
Transmission from person to person
Transmission can also occur from person to person, with cases reported in caregivers for sick individuals and in health care settings.
Available data indicates that respiratory secretions are likely an important aspect of person-to-person transmission, with Nipah virus readily identified in the saliva of infected patients and patients with respiratory symptoms being more likely to transmit the virus. There is some evidence that being present in the room with a Nipah virus patient with no physical contact is a risk factor for infection, indicating the likelihood of aerosol transmission.
Several outbreak investigations reveal risk factors for transmission among caregivers include close physical contact, sharing beds, and sharing utensils and food, indicating transmission through direct contact.
What infection prevention and control measures are important to protect nurses and prevent Nipah virus spread in health care facilities?
Public health experts call attention to the importance of primary prevention to reduce the potential for Nipah virus spillover into humans, such as reducing the risk of bat to human transmission by preventing bat access to date palm syrup and other fresh food products, reducing the risk of animal to human transmission by using PPE when working with sick animals, and reducing the risk of person-to-person transmission by avoiding close contact with sick individuals and providing early health care and supportive care.
Health care employers are responsible for providing a safe work and patient care environment. Multilayered infection prevention measures should be implemented in all health care facilities when Nipah virus is suspected or confirmed:
- Patient screening – Screen patients for Nipah virus-like illness, especially among those with exposure or who have recently traveled to an area with a known or high risk for an outbreak. Provide education and training to staff on recognizing and responding to Nipah virus infections.
- Isolation and source control – Patients with suspected or confirmed Nipah virus infection should be isolated promptly in an airborne infection isolation room (AIIR).
- Ventilation – Adequate ventilation is also essential for reducing the risk of Nipah virus transmission in lobbies, waiting rooms, and other areas of the facility where a suspected or confirmed case could be present before being identified and isolated.
- Personal protective equipment – Health care workers caring for patients with suspected or confirmed Nipah virus infections should wear a powered air-purifying respirator (PAPR), coveralls impervious to viral penetration with head and shoe coverings, and gloves.
- Exposure notification and contact tracing – Employers should conduct contact tracing and immediately notify staff who were potentially exposed. Exposure should include both direct contact while providing care and sharing air space (e.g., being in the same waiting room, triage station, etc.).
- Paid precautionary medical removal – Employers should provide paid precautionary medical removal for any health care worker who is removed from the workplace due to occupational exposure or infection with Nipah virus.
References
- World Health Organization. Nipah virus. January 29, 2026. https://www.who.int/news-room/fact-sheets/detail/nipah-virus
- Ganguly, A., Mahapatra, S., et al. The rising threat of Nipah virus: a highly contagious and deadly zoonotic pathogen. Virology Journal, 2025, 22(139). https://link.springer.com/article/10.1186/s12985-025-02728-4
- Luby, S.P, Gurley, E.S., and Jossain, M.J. Transmission of Human Infection with Nipah Virus, in Improving Food Safety Through a One Health Approach: Workshop Summary. Institute of Medicine, 2012. https://www.ncbi.nlm.nih.gov/books/NBK114486/
- Pritchard, S. and Hornsey, E. The role of infection prevention and control in the mitigation of human-to-human transmission of Nipah virus: a systematic review. Antimicrobial Resistance & Infection Control, 2026, 15(1). https://link.springer.com/article/10.1186/s13756-025-01677-5